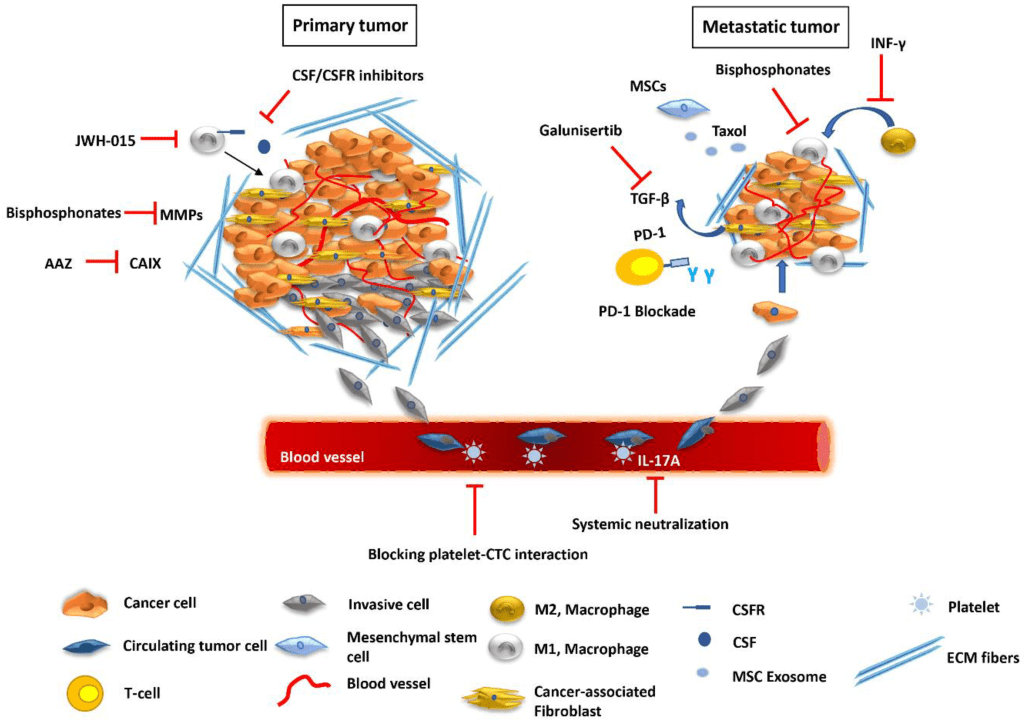
Introduction:
Cancer is not just a disease of uncontrolled cell growth, it’s a complicated biological process that is affected both by the cancer cells and their environment. Beyond the cells, or tumor microenvironment (TME), is the key to why cancer appears, advances, and is treated. In recent years, there has been a shift in the paradigm of oncology: the researchers and clinicians are interested in the cancer cells as well as exploring the microenvironment Role in cancer therapy. The TME can be discovered to treat cancer and improve existing therapies by understanding and manipulating.
What is the Tumor Microenvironment?
The tumor microenvironment is the most complex interaction of cells around cancer cells. It includes:
– Stromal cells (fibroblasts, adipocytes, pericytes)
– Immune cells (T-cells, macrophages, neutrophils, dendritic cells)
– Blood vessels and lymphatics
– Extracellular matrix (ECM)
– Signaling molecules (cytokines, growth factors, enzymes)
All these components interact continuously with cancer cells to create a dynamic system that continuously changes with progressing tumor development.
How the Microenvironment Impacts Cancer Treatment
Drug Resistance
The TME contributes in several ways:
– Hypoxia (oxygen depletion), which occurs commonly in solid tumors, is a hindrance to the activity of radiation and some chemotherapy agents.
– The ECM acts as a physical barrier to entry by drugs.
– CAFs and immune cells can secrete pro-survival factors that enable tumor cells to be resistant to therapy.
Immune Evasion
The immune system helps in destroying cancer cells. The TME, however, can inhibit the immune system by:
– Overexpressing immune checkpoint molecules like PD-L1, which “switch off” T-cell function.
– This immunosuppressive niche limits the effectiveness of immunotherapies unless treated specifically.
Angiogenesis and Vascularization
It is leaky and disordered vessels that are also a brake on therapeutic drug delivery. Anti-angiogenic treatments such as VEGF inhibitors are crafted to regularize tumor vasculature in an attempt to maximize the effectiveness of treatment.
Therapeutic Strategies Targeting the Tumor Microenvironment
With scientists turning to the microenvironment for cancer treatment, many targeted strategies have emerged:
Immunotherapy Augmentation
Anti-PD-1 and anti-CTLA-4 checkpoint inhibitors have revolutionized cancer treatment. However, their potential is frequently limited by immune-suppressive TME. Mechanisms to overcome this hurdle are:
– Depleting Tregs or MDSCs
– Use of cytokine therapy (e.g., IL-2 or IFN-γ) to stimulate immune cells
– Customized vaccines for augmentation of anti-tumor immunity
Anti-Angiogenic Therapy
Targeted agents such as bevacizumab infiltrate starved tumors by suppressing angiogenesis, and the formation of new blood vessels. New strategies, however, infiltrate vascular normalization reorganizing vasculature abnormalities to improve drug and oxygen delivery and eventually maximize the efficacy of chemo- and radiotherapy.
Targeting CAFs and ECM Remodeling
Cancer-associated fibroblasts reorganize the ECM to support growth and drug resistance. Abrogation of the activity of CAFs or interference with certain elements of the ECM can enhance drug penetration and decrease cancer cell survival.
Modulation of Hypoxia
Strategies for targeting tumor hypoxia are:
– Oxygen delivery enhancers
– Hypoxia-activated prodrugs (activated in low-oxygen regions)
– Gene therapy against hypoxia-inducible signaling pathways
Reprogramming of the TME
Reprogramming the TME to a pro-tumor rather than an anti-tumor environment is a new idea. This includes
– Re-seeing tumor-associated macrophages (TAMs) from tumor-promoting (M2) to tumor-removing (M1) phenotype
– Modulating the metabolic interaction in the TME, e.g., glucose and amino acid supply, to suppress cancer cell survival
Future Directions and Challenges
While TME-targeted therapy holds a lot of promise, there are some challenges:
– Heterogeneity: The composition of the microenvironment varies with the nature of the tumor and even among different parts of a tumor.
– Biomarkers: It is crucial to identify consistent biomarkers for response expectation to TME-directed therapy.
– Resistance mechanisms: Tumors cause resistance by upregulation of other pathways.
However, with recent advances in single-cell sequencing, AI-based analytics, and 3D tumor modeling, the future of precision cancer therapy with TME modulation appears promising.
Conclusion:
The old dogma of cancer therapy is breaking down. Today, exploring the microenvironment’s role in cancer treatment is not a scientific luxury anymore but a clinical necessity. Not just the tumor but its natural habitat has to be targeted for a more integrated and efficient treatment. With immunotherapy, anti-angiogenic agents, and metabolic reengineering, TME-targeting strategies have the potential to shatter resistance, optimize the therapeutic response, and optimize the survival of patients. As the investigation goes deeper, so does our ability to outwit cancer at all levels.
FAQs
- What is the tumor microenvironment (TME)?
The tumor microenvironment consists of the non-cancerous cells and tissues that surround a tumor, including immune cells, fibroblasts, blood vessels, extracellular matrix, and signaling molecules. It plays its most powerful role in tumor growth, metastasis, and treatment.
- Why is tumor microenvironment important in cancer therapy?
The TME can affect tumor sensitivity to treatment by drug resistance, giving rise to cancer survival and inhibiting immunity.
- What is the role of immune cells in the TME in cancer therapy?
Some of the immune cells found in the TME, including regulatory T cells and myeloid-derived suppressor cells, can suppress the body’s anti-cancer immunity. Inhibition of them will make immunotherapies more effective.
- What are some examples of TME-targeting therapies?
Examples include immune checkpoint inhibitors (e.g., anti-PD-1), anti-angiogenic agents (e.g., bevacizumab), CAF inhibitors, hypoxia-targeted therapy, and extracellular matrix remodeling agents.
- What are the difficulties in targeting the tumor microenvironment?
These difficulties include tumor heterogeneity, the issue of predictive biomarker identification, and the development of resistance mechanisms. Investigations are currently addressing these issues to improve the therapeutic effect of TME-targeted therapy.